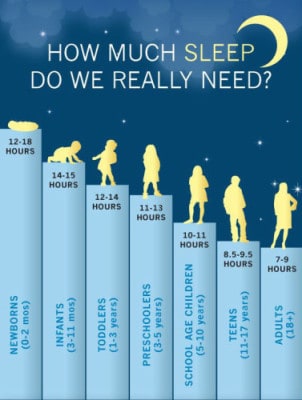
How many hours of sleep is enough?
Behind the ever increasing business productivity in this new economy, there is a seemingly gradually erosion of our sleeping time. In addition to the multitude of family needs, there is hardly any time left for taking care of our personal well being such as exercise and leisure time that is essential to maintain our good health. Many of us, therefore, are looking for the “optimal” amount of sleep, i.e. the minimal amount of sleep a night without compromising our general well being.
Before providing an answer to this surprisingly complex question, it’s worth taking the time to review the science of health outcomes as they relate to sleep. Sleep affects many aspects of health and function. There are three broad categories: cognitive, mental/behavioral, and physiologic. Cognitive function includes such processes as memory, learning, and abstract reasoning; whereas mental/behavioral health can include general quality-of-life indicators and risks for such specific diagnoses as anxiety or depression. The category of general physiology includes appetite, weight gain, and metabolism, along with the processing of carbohydrates (yes, not enough sleep can make you fat!), and its effects on cardiovascular health.
The National Sleep Foundation recently published some age-based recommendations for nightly sleep duration. A quick glance at the abstract confirms what we already know—adults should be targeting 7-9 hours per night. But on these adult targets, a new category has been created—6 hours per night “may be appropriate” for adults. The questions are: In what situations are 6 hours appropriate, for how long, and for whom? The stakes are fairly high. From 10% to 30% of the US adult population sleeps fewer than 6 hours per night. Unfortunately, the new recommendations, as currently published, don’t provide much detail on this point.
There are also recent data to suggest that susceptibility to sleep debt exhibits “trait-like” characteristics, meaning that individuals have an inherent ability (or lack thereof) to perform well under varying amounts of sleep restriction. Translation—”one person 6 or even 5 are another’s 8 hours per night for optimal performance on a given task.” Do trait-like characteristics in the response to chronic sleep deprivation extend to physiologic effects, such as weight gain or appetite change? One would assume that they do, but this area hasn’t been well studied. We simply know that these physiologic changes are more common in patients who sleep fewer than 7 hours per night.
Recommending a specific duration of sleep for a specific individual, needless to say, is problematic for healthcare practitioner given no well-studied guidelines to follow. In my practice, I used 6 hours as the minimal baseline and assess patient’s individual trait during our initial and subsequent visits. It is essential to discuss with the patient on their sleeping hygiene such as emphasizing bedroom is strictly for sleeping, intimacy and maybe some light reading only. Daily practice of relaxation techniques such as meditation and exercise are highly recommended. Many studies have shown a “power nap” as little as 15-minutes during the day is a much better remedy to re-charge the day than caffeine drink and may offer other health benefits. Given the potential dependence nature of sleeping medications, they should always be the last resort and should be used only for a short period of time to break the insomnia viscous cycle. More importantly, sleeping is becoming another vital sign of our well being given now we have a better understanding of the cognitive, mental and the likely increased physiological and cardiovascular risks.